Why This Topic Matters in Massachusetts
By mid-winter in Massachusetts, the holidays are long over, daylight is limited, and cold weather has settled in for months. For many people, this is also when mood drops, motivation fades, and alcohol or drug use starts creeping up.
If you’ve noticed that your substance use increases during winter—or that a loved one struggles more this time of year—you’re not imagining it. The connection between winter depression and substance use in Massachusetts is real, well-documented, and more common than many people realize.
Many individuals seeking help at Real Recovery Centers in Chelmsford describe the same pattern: winter brings isolation, low energy, and emotional numbness, and substances begin to feel like relief. Understanding why this happens is often the first step toward breaking the cycle and getting the right kind of support.
Understanding Winter Depression and Seasonal Affective Disorder (SAD)
Winter depression isn’t just disliking cold weather. For some people, it meets the criteria for Seasonal Affective Disorder (SAD)—a form of clinical depression that follows a seasonal pattern.
Why New England Winters Hit Especially Hard
Massachusetts sits at a northern latitude where winter brings:
- Short daylight hours
- Frequent cloud cover
- Limited exposure to natural sunlight
- Reduced outdoor activity
Sunlight plays a key role in regulating brain chemistry. When light exposure drops, serotonin (which helps regulate mood) decreases, while melatonin (which affects sleep) increases. This disrupts circadian rhythms—the body’s internal clock—leading to fatigue, low mood, and sleep changes.
Common Symptoms of Winter Depression
Winter depression can look different for everyone, but often includes:
- Persistent low mood or emotional numbness
- Low energy or oversleeping
- Changes in appetite or cravings
- Social withdrawal
- Difficulty concentrating
- Loss of interest in activities
When these symptoms appear every winter and interfere with daily life, it’s more than “winter blues.”
The Connection Between Winter Depression and Substance Use in Massachusetts
If you’ve noticed your drinking increases between November and March, you’re asking the right question.
The answer lies in how depression, environment, and coping strategies interact.
Why Substances Feel Helpful at First
When winter depression sets in, substances may feel like they:
- Lift mood temporarily
- Increase energy
- Reduce emotional pain or anxiety
- Help pass time during isolation
This is known as self-medication. The relief is real—but short-lived.
Alcohol is a depressant, and many drugs disrupt sleep and brain chemistry. Over time, substance use worsens depression rather than relieving it.
The Role of Isolation and Structure Loss
Winter limits social interaction and routine. Fewer activities, canceled plans, and weather-related isolation create long stretches of unstructured time—one of the biggest risk factors for increased substance use.
Alcohol and substance use often increase in winter due to seasonal depression affecting mood, energy, and brain chemistry. Reduced sunlight disrupts serotonin and sleep cycles, leading many people to self-medicate. While substances may provide temporary relief, they ultimately worsen depression and increase dependence, creating a reinforcing cycle.
The Dangerous Cycle: How Depression and Substance Use Reinforce Each Other
Winter depression and substance use don’t just coexist—they actively fuel one another.
- Winter depression brings low mood, fatigue, and isolation
- Substances are used to cope or feel relief
- Sleep, motivation, and emotional regulation worsen
- Guilt, shame, or consequences increase
- Substance use escalates to cope with worsening depression
In Massachusetts, this cycle often becomes more difficult during the darkest winter months, especially when low light and isolation persist. Without added support or intentional coping strategies, it can be hard to interrupt.
Warning signs include:
- Drinking or using more in winter than other seasons
- Mood worsening after substance use
- Increasing isolation
- Difficulty functioning at work or home
- A history of winter relapse
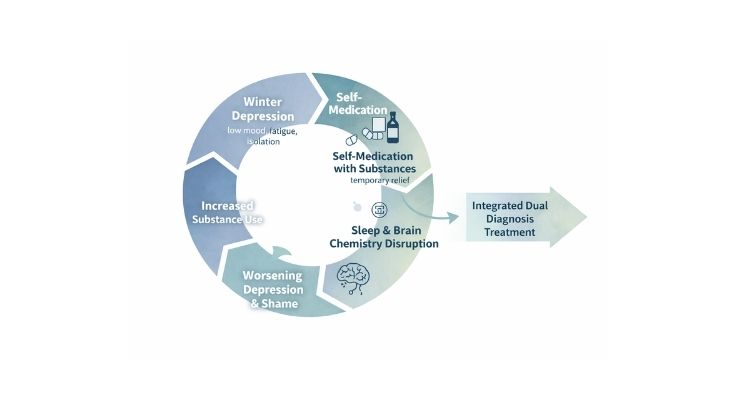
Why Treating Both Conditions Together Is Essential
Treating substance use without addressing depression leaves a major relapse risk unaddressed. Treating depression while substance use continues often limits progress.
Integrated dual diagnosis treatment addresses both conditions at the same time using coordinated care.
This may include:
- Cognitive Behavioral Therapy (CBT) to address depressive and addictive thought patterns
- Dialectical Behavior Therapy (DBT) for emotional regulation
- Medication management when appropriate
- Structured programs such as PHP or IOP, depending on severity
Massachusetts residents comparing care levels can explore structured outpatient treatment options or integrated addiction treatment programs statewide for guidance.
Coping With Winter Depression Without Substances
These strategies support recovery but don’t replace professional care when both depression and substance use are present.
Light and Routine
- Use a 10,000-lux light box each morning
- Open blinds immediately upon waking
- Maintain consistent sleep and meal times
Movement and Connection
- Short walks or gentle indoor movement
- Virtual or in-person recovery groups
- Scheduled check-ins with supportive people
Professional Support
- Continue therapy through winter
- Increase support during high-risk months
- Develop a winter relapse prevention plan
Articles on how substances affect mental health long-term and understanding drug withdrawal symptoms can also help clarify what’s happening in your body and brain.

Frequently Asked Questions
Can winter depression cause relapse?
Yes. Seasonal depression reduces motivation and coping capacity, increasing relapse risk without added support.
Is it normal to drink more in winter?
It’s common, but increased use may signal underlying depression or a developing cycle that needs attention.
What treatment works best for both conditions?
Integrated dual diagnosis treatment that addresses mental health and substance use together.
Does insurance cover treatment in Massachusetts?
Most plans, including MassHealth and private insurance, cover dual diagnosis care. Verification is usually available.
Support Is Available—Even in the Middle of Winter
Winter depression and substance use are closely connected, especially in Massachusetts. Both are treatable, and waiting for spring isn’t necessary—or helpful.
If you or someone you love is ready to begin recovery, the Chelmsford team at Real Recovery Centers is here to help. Call today to verify insurance or learn more about treatment options designed for co-occurring depression and substance use.
Recovery is possible, even in the coldest months. If you’re considering support, our Chelmsford team can help you understand outpatient options and next steps.




