Addiction rarely exists in isolation. Clinical research and outpatient experience consistently show that many people seeking addiction treatment have lived through trauma, chronic stress, or adverse experiences that shape how they cope. Research consistently shows that trauma is common among people seeking addiction treatment, making it an essential consideration in effective care.
Across Massachusetts, individuals, families, and healthcare professionals are seeking treatment models that address both trauma and substance use without judgment. In Chelmsford, Real Recovery Centers integrates trauma-informed principles into evidence-based outpatient care, offering a clinically grounded approach that supports long-term stability without retraumatization.
This guide explains what trauma-informed care is, why it matters in addiction treatment, and how different treatment options compare for people with trauma histories.
What Is Trauma-Informed Addiction Treatment in Massachusetts?
Trauma-informed care is a framework that acknowledges how common trauma is among people seeking addiction treatment. Instead of focusing on what is “wrong,” it centers on understanding what someone has experienced and how those experiences continue to affect behavior, emotions, and recovery.
According to Substance Abuse and Mental Health Services Administration (SAMHSA), trauma-informed addiction treatment Massachusetts providers follow six core principles:
- Safety – creating physical and emotional environments where people feel secure
- Trustworthiness and transparency – clear expectations and consistent communication
- Peer support – healing through shared lived experience
- Collaboration and mutuality – clients as active partners in treatment
- Empowerment, voice, and choice – honoring autonomy and personal goals
- Cultural and historical awareness – recognizing identity, background, and systemic factors
These principles guide how treatment is delivered, from therapy sessions to program structure, reducing the risk of triggering trauma responses during care.
The Connection Between Trauma and Addiction
Many people in Massachusetts who seek addiction treatment have experienced trauma at some point in their lives. This may include childhood neglect, abuse, violence, sudden loss, or medical trauma. Understanding this connection helps explain why relapse risk is higher when trauma goes unaddressed.
Trauma-informed care often overlaps with dual diagnosis outpatient treatment, which addresses substance use alongside co-occurring mental health conditions rather than treating them separately.
How Trauma Affects the Brain and Nervous System
Neuroscience research has demonstrated that trauma can affect emotional regulation and stress response systems. When the nervous system remains in a heightened state of alert, everyday stress can feel overwhelming.
- In trauma survivors, the amygdala—the brain’s threat-detection center—can remain hyperactivated, scanning for danger even in safe environments. This constant vigilance strains the nervous system and makes emotional regulation much harder, which is why some people turn to substances that temporarily quiet the brain’s alarm response.
- The prefrontal cortex, which supports decision-making and impulse control, may be less effective under stress
- The hippocampus, involved in memory and regulation, may struggle to organize traumatic memories
Substances often temporarily reduce these symptoms, which is why they can feel helpful at first. Over time, however, substance use worsens emotional regulation and deepens dependency.
Trauma can change how the brain responds to stress and emotional cues. When someone has experienced trauma, areas of the brain involved in threat detection, emotional regulation, and memory may become dysregulated. This can make everyday stress feel overwhelming and increase vulnerability to substance use as a way to cope. The illustration below shows how trauma can affect key brain regions commonly involved in addiction and recovery.
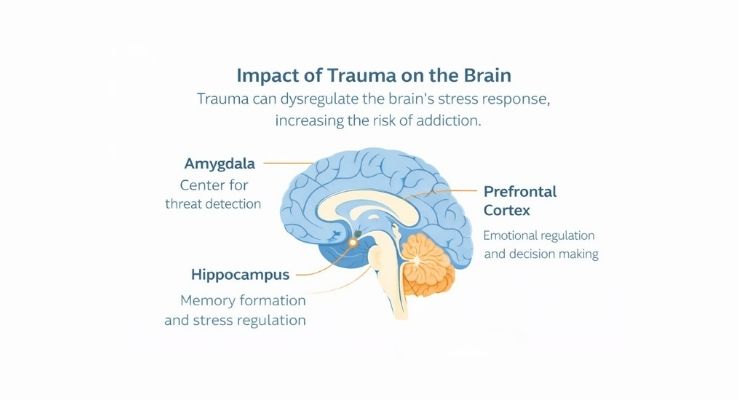
How Trauma Leads to Addiction
Trauma can dysregulate the brain’s stress response, making emotions feel overwhelming or unsafe. Substances are often used to cope with this distress, increasing the risk of addiction when trauma remains untreated.
Why Trauma-Informed Care Is Essential for Lasting Recovery
Traditional addiction treatment models sometimes rely on confrontation, rigid rules, or limited client choice. For people with trauma histories, these approaches can unintentionally recreate feelings of powerlessness or threat.
Trauma-informed addiction treatment Massachusetts programs aim to:
- Reduce relapse linked to trauma triggers
- Improve emotional regulation skills
- Increase treatment retention and engagement
- Support co-occurring disorders, including trauma-related mental health conditions and substance use
Integrated treatment approaches have been associated with improved engagement and reduced relapse risk, particularly when trauma and substance use are addressed together rather than separately. This is why trauma-informed principles are woven throughout outpatient levels of care.
Comparing Trauma-Informed Treatment Options in Massachusetts
Choosing the right level of care depends on symptom severity, daily responsibilities, and personal support systems. Below is a comparison of common outpatient options using trauma-informed principles.
Partial Hospitalization Program (PHP)
PHP provides the highest level of outpatient structure, with daily therapeutic programming while allowing individuals to live at home.
Best for
- Significant trauma symptoms
- Early recovery needing stabilization
- Difficulty managing emotions or triggers
Considerations
- Requires a larger time commitment
- Less scheduling flexibility
Learn more about the structure and benefits of a Partial Hospitalization Program in Massachusetts.
Half-Day Treatment Program
Half-Day treatment offers intensive therapeutic support with more flexibility than PHP, making it suitable for individuals balancing recovery with work or family responsibilities.
Best for
- Moderate trauma symptoms
- Step-down care after PHP
- Need for structured support without full-day programming
Considerations
- Less daily structure than PHP
Explore how a Half-Day Treatment Program supports trauma-informed recovery.
Outpatient Program (OP)
OP provides ongoing therapy and support with the greatest flexibility. It is often used for continued recovery or long-term support.
Best for
- Stable recovery
- Established coping skills
- Strong external support systems
Considerations
- Requires self-management between sessions
Learn more about Outpatient Rehab in Massachusetts.
Evidence-Based Therapies Used in Trauma-Informed Addiction Treatment
Trauma-informed programs rely on therapies that emphasize safety, skill-building, and empowerment.
- Dialectical behavior therapy (DBT) in Massachusetts helps people manage intense emotions, distress tolerance, and emotional regulation in trauma-informed recovery settings. Learn how DBT supports emotional regulation in Massachusetts recovery settings.
- Cognitive Behavioral Therapy (CBT) addresses trauma-related thought patterns that fuel substance use.
- Motivational Interviewing (MI) respects autonomy and helps individuals build internal motivation for change.
Education around medication safety and substance interactions is also essential. For example, understanding the risks of combining gabapentin and hydrocodone can prevent unintended harm during recovery.
What to Expect From Trauma-Informed Addiction Treatment in Massachusetts
Treatment begins with a comprehensive assessment conducted at a comfortable pace. Trauma history is explored gently, with full respect for personal boundaries.
Key elements include:
- Clear communication and predictable structure
- Choice around participation and pacing
- Skill development before deep trauma processing
- Integrated care for co-occurring mental health conditions
Clients are never pressured to disclose details before they feel ready.
Frequently Asked Questions
What is trauma-informed addiction treatment?
Trauma-informed addiction treatment recognizes the impact of trauma and prioritizes safety, choice, and collaboration throughout recovery.
Do I need PTSD to benefit from trauma-informed care?
No. While PTSD is one manifestation of trauma, trauma-informed care can benefit anyone who has experienced overwhelming stress, loss, neglect, medical trauma, or adversity, even without a formal diagnosis. Many people who don’t identify as having PTSD, or who experience post-traumatic stress symptoms, find trauma-informed approaches especially helpful because the care feels safer, more respectful, and more responsive to their lived experience.
Is trauma-informed care available in outpatient programs?
Yes. Many Massachusetts outpatient programs, including PHP, Half-Day, and OP, integrate trauma-informed principles.
Does insurance cover trauma-informed addiction treatment in Massachusetts?
Most insurance plans, including MassHealth and private insurance, cover evidence-based outpatient addiction treatment. Coverage varies by plan.
How do I know if this approach is right for me?
If previous treatment felt overwhelming or ineffective, or if emotional triggers play a role in substance use, trauma-informed care may be a better fit.
Finding Care That Feels Safe and Effective

Addressing addiction alongside trauma creates a stronger foundation for recovery. Trauma-informed addiction treatment Massachusetts programs offer a path that respects resilience while supporting meaningful change.
If you or someone you love is ready to begin recovery, our Chelmsford team is here to help. You can speak with our Chelmsford team to verify insurance or learn more about your treatment options.
Our team can help you explore outpatient addiction treatment options designed to support recovery with safety, dignity, and flexibility.





